Hypertrophy of the palatine tonsils and the pharyngeal tonsil is a problem that particularly affects children - younger and older. In order for a diagnosis to be made well, an appropriate diagnostic procedure is required to confirm or rule out suspicions of pathology. There are a number of examinations that can be used, but not all of them are sufficiently reliable, the reason for which may be, for example, the young patient's unwillingness to cooperate with the doctor.
The system of lymphatic tissue clusters located at the border of the airway and digestive tract is called Waldeyer's ring, and includes elements such as the palatine tonsils, the pharyngeal tonsil (the so-called third tonsil), the lingual tonsil, the tonsils of the trochlea, the lymphatic bands and scattered lymph nodules on the posterior pharyngeal wall. The palatine tonsils are the largest component by volume, and these show activity on contact with antigen - clusters of proliferation (a demarcated lymphatic tau) appear and disappear after about three weeks of contact with the antigen, the proliferation centres themselves being nothing more than clusters of lymphocytes. The tonsils are characterised by very high concentrations of immunoglobulins, higher than those recorded in the spleen or lymph nodes, and their structure allows them to be classified as lymphoid organs, forming part of the immune barrier that protects us from food and respiratory antigens [1].
The debatable role of the palatine tonsils
The role of the palatine tons ils is a controversial issue in the deliberations of many specialists - they are assumed to be a barrier element of the human organism, an element of defence against microorganisms entering the organism through food and inhalation. On the other hand, however, they can be a source of serious danger for the organism - when pathological changes occur in their area, which usually takes place in a situation of chronic inflammation. Such abnormalities may become a causative element in the pathogenesis of many conditions, including rheumatic, inflammatory glomerulonephritis, endocarditis and autoimmune diseases. Indeed, studies to date have noted statistically more frequent circulating immune complexes in individuals with tonsillar pathologies [1].
Diagnostic process
The start of the examination is always the medical history, which should give the specialist information on the frequency of rhinorrhoea, periods of nasal obstruction, snoring, sleeping with the mouth open, past history of acute tonsillitis. Information on middle ear infections or episodes of pain in this area is also important. Parents will be asked about their observations of their child's behaviour and functioning in the context of the suspected hearing loss (turning up the TV, articulation problems, learning difficulties) [1].
The next stage is an ENT examination, which includes an oral and pharyngeal examination, anterior and posterior rhinoscopy, and palpation (touch) of the neck [1].
Rhinoscopy is an examination that allows visual assessment of the nasopharyngeal structures, as well as secretions, nasal mucosa, the appearance of the nasal auricles including the septum, and the presence of pathological changes (nodules or polyps) [4].
The above-mentioned examination procedures are complemented by tympanometric testing [1]. Tympanometry is the measurement of the acoustic immittance of the ear as a function of air pressure in the ear canal. The term 'immittance' is a general term referring to both impedance (the acoustic resistance posed by a sound-conducting structure to the flow of acoustic energy) and admittance (the inverse of impedance - the susceptibility of a structure to acoustic energy flow) [3].
These tests are a standard diagnostic procedure, the starting point for further management. It is therefore essential that all patients undergo this part, regardless of age.
Endoscopic examination
The third tonsil is a structure that remains invisible when viewing the throat and only an ENT specialist is able to assess its structure. Visual assessment is possible in a number of ways, namely - finger examination, which is definitely unpleasant for the child and, moreover, through the child's lack of cooperation, can also be unreliable and give an unreliable result. Another way is examination with a specialised mirror, which also requires the child to cooperate and remain calm during the examination. If it is not possible to examine the tonsil in this way, an X-ray may be taken, which exposes the child to a dose of radiation. A solution may be an examination performed with an endoscope - relatively easy to perform, giving high reliability, safe and comfortable for the young patient. The examination procedure involves only inserting a thin, flexible endoscope into the nose or a high-angle endoscope into the mouth [2].
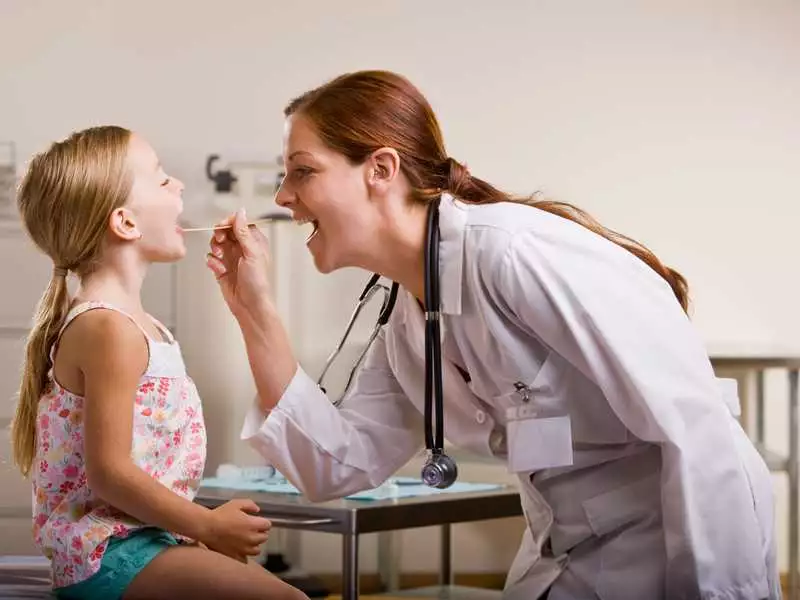
photo: panthermedia
As can be seen, most of the examinations can be cumbersome to perform, due to the fact that they require the patient's cooperation. Young children, in relation to unpleasant sensations such as finger or mirror examination, are not cooperative. Examination with an endoscope is non-invasive and does not require special cooperation from the child, hence it is an examination that can be successfully applied even in younger children.